A spinal cord injury can flip your world upside down in seconds. Suddenly, things you took for granted, like moving your legs, standing, and even just feeling steady, become huge challenges.
You naturally look for anything that might bring some movement or freedom. Epidural stimulation for spinal cord injury may give you the freedom you are looking for.
What is it?
It uses carefully targeted electrical pulses on the nerves below the injury to help you get some lost abilities back. If you want to walk a little steadier, move your arms better, or simply enjoy life more, it is the option you should opt for.
To figure out if this is the right path, you need to know how epidural stimulation works, who stands to gain from it, and what’s actually possible. That’s how you make smart, confident choices about your treatment.
Wondering if epidural stimulation is the right option for your specific spinal cord injury? Every case is different, and expert evaluation is essential before making any decision. MedicoExperts can connect you with leading neurosurgeons and top hospitals in India for a detailed medical opinion.
What is Epidural Stimulation for Spinal Cord Injury?
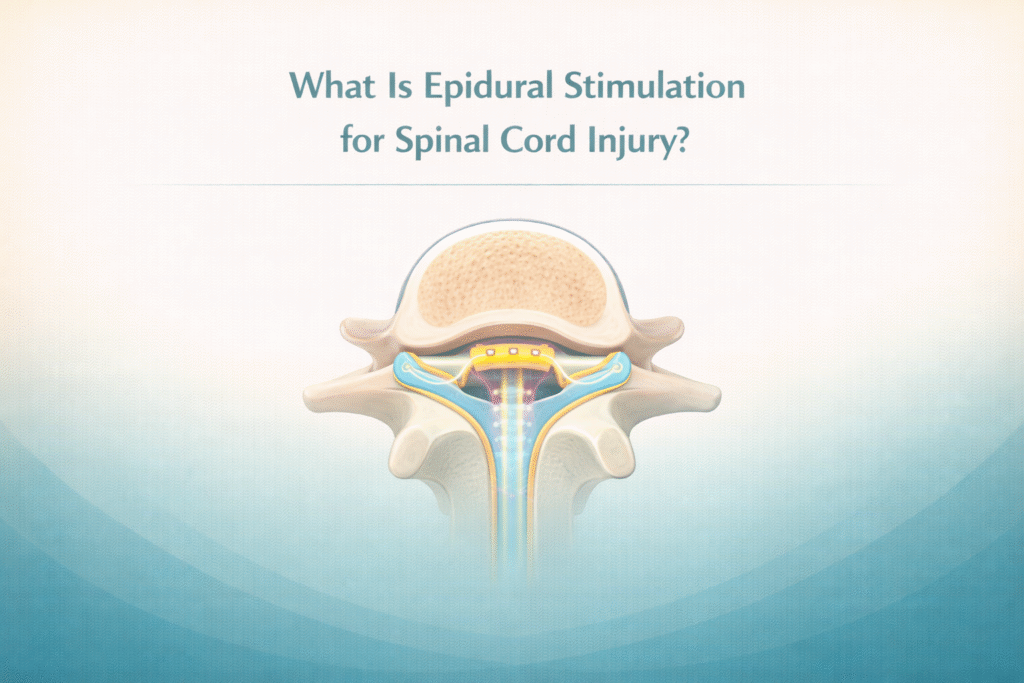
Epidural stimulation for spinal cord injury is promising for people recovering from such injuries. It’s not a cure for paralysis, but it does offer a new way to work with the nervous system and maybe bring back the abilities that were lost.
To see why this matters, you have to know what the therapy is all about and how it stands apart from the usual treatments.
What is it & Basic Mechanism?
Epidural stimulation is a procedure where tiny electrical signals are sent directly to certain spots on the spinal cord using an implanted device. Doctors put electrodes in the epidural space, just outside the spinal cord, and those electrodes deliver gentle pulses that can jump-start nerve activity below the injured area.
Basically, these impulses help “wake up” spinal circuits that might still be there but aren’t working after an injury. Even if the brain can’t send messages down because of the damage, a lot of the wiring inside the spinal cord itself still reacts when you give it a nudge. By tweaking the strength and timing of those signals, doctors try to make those circuits more responsive.
This approach isn’t like the usual treatments for spinal cord injuries, which mostly deal with rehab, avoiding complications, or using assistive gadgets. Epidural stimulation goes right for the neural pathways, aiming to get them moving again. It’s meant to work alongside rehab, not take its place.
How Epidural Stimulation Helps Spinal Cord Injury Recovery?
Epidural stimulation works because the spinal cord has its own complex network of nerves that can still create movement patterns, even after an injury. By sending electrical signals to these networks, the stimulation makes them more responsive.
That way, even weak signals from the brain, or small voluntary efforts, can sometimes trigger real movement.
Studies show that some people with spinal cord injuries experience better voluntary movement, steadier standing, improved control over heart rate and blood pressure, and even better bladder or bowel function after epidural stimulation.
The results aren’t the same for everyone, and the progress depends on the kind of training people do during rehab, and the benefits usually show up in specific tasks rather than across the board.
For example, two people are getting epidural stimulation. One stands up or manages a few assisted steps in therapy. On the other hand, another gets better at sitting up straight or controlling their legs.
It comes down to how hard and how often you train in rehab. If someone spends more time working on walking, they usually get better at stepping.
But if they put their energy into core exercises, their balance while sitting improves instead. The thing is, the progress tends to stick to whatever they’re practicing. So if someone gets better at walking, it doesn’t mean their hands suddenly work better, too. The results are specific to the skills they train.
This therapy isn’t right for everyone. Whether you are a good candidate depends on things like where and how severe your injury is, your general health, what you hope to achieve, and a specialist’s assessment.
Doctors need to take a close look before starting treatment to figure out if it makes sense and what’s actually possible.
Epidural Stimulation Surgery: The Treatment Process
Epidural stimulation starts with thorough evaluations, moves on to a precise surgery, and then shifts into a long stretch of rehab.
Every step in this procedure matters. Each one shapes how safe the procedure is for you and what results you can expect.
Pre-Surgery Evaluation
The Surgical Procedure
Post-Surgery Recovery and Rehabilitation
Eligibility for epidural stimulation depends on multiple medical factors, and the assessment process can feel overwhelming. Our care team helps you consult the right specialists, choose reputed hospitals, and organize medical visits, documentation, and travel support.
Epidural Stimulation Success Rate & Recovery Outcomes
Epidural stimulation has become popular lately, especially for people recovering from spinal cord injuries. That’s because results do vary from person to person. Still, when you look at both the research and what actual patients say, you start to get a sense of what’s possible and what gets in the way.
Clinical Success Rates
Some studies show that, for certain people, epidural stimulation can spark real neurological and functional changes. People report things like better voluntary muscle movement, being able to stand with some help, and even more precise control over specific tasks.
People with incomplete spinal cord injuries usually see better results than those with complete injuries, mostly because they’ve still got some neural connections left.
So, what kinds of changes do people notice? You’ll hear about stronger core stability, muscles that wake up and respond better, more stable blood pressure, and sometimes, even a bit of voluntary movement.
But let’s be clear, epidural stimulation isn’t a magic fix. Not everyone experiences the same gains, and the real progress tends to happen when rehab and stimulation go hand in hand.
Real Patient Recovery Stories
Progress isn’t always about standing or walking. Take Stefanie, for example. She lived with a high cervical spinal cord injury and battled dangerously low blood pressure for years. Then she joined a research study using spinal cord epidural stimulation. Suddenly, things started changing. Her body’s automatic functions kicked in again. Now she can eat on her own, get her service dog ready, and even drive without worrying she’ll lose consciousness. For her, that’s a huge leap in quality of life.
Vishnu Agarwal is 48 and lives in India. After a C7 spinal cord injury, he spent months looking into every possible option. In the end, he packed his bags for Bangkok, chasing a shot at epidural spinal stimulation and some intense physiotherapy.
Just a week after surgery, something shifted. For the first time since his accident, he managed to stand. He needed a hand, but still, he stood. His legs started moving better, and he found it way easier to sit up without wobbling.
Stories like Vishnu’s really show what epidural stimulation can do. It’s not some miracle cure, but it makes a real difference. People get to stand again with help, or they start moving in ways they thought were gone for good.
Factors Affecting Success
Several factors play a significant role in determining the outcomes of epidural stimulation:
- Injury Severity and Location: Preserved neural circuits enhance responsiveness to stimulation.
- Time Since Injury: Both acute and chronic injuries may respond, though the degree of neural adaptability can differ.
- Patient Age and Overall Health: The general state of health of the patient is also an important factor.
- Commitment to Rehabilitation: In some cases, consistent therapy can be very important.
Due to the difference in outcome, you need to have realistic expectations and assessment in your decision-making process for epidural stimulation in your recovery plan.
Epidural Stimulation Cost: Investment and Affordability
Let’s break down what you’re actually paying for with epidural stimulation (or spinal cord stimulator implants), both in India and around the world, and why the prices swing so much.
Cost Breakdown in India
Epidural Stimulation Cost in India: India vs International
Financing and Insurance Options
Long-Term Costs
Epidural Stimulation Treatment in India: Top Centers & Expertise

India is now a go-to spot for cutting-edge epidural stimulation and spinal cord stimulator treatments. You get skilled doctors, modern hospitals, and prices that won’t wipe out your savings. If you’re thinking about coming to India for this kind of therapy, here’s the real story:
Why Choose India for Epidural Stimulation?
The biggest cities, Delhi, Mumbai, Bangalore, Chennai, and Gurugram, are packed with specialist centers. These places have teams of neurosurgeons and pain experts who know neuromodulation inside out, whether you need spinal cord or epidural stimulation. The hospitals use up-to-date imaging and surgical tech, so device implantation is precise and safe.
Honestly, the price difference is huge. Treatments here cost way less than in most Western countries, but you still get great care. For a lot of people, it has changed their lives. It opens doors to therapies they couldn’t afford elsewhere.
Indian centers with good reputations show strong results. Most patients see major pain relief and better function compared to where they started. The numbers back it up.
What to Look for in a Treatment Center?
Look for centers with board-certified neurosurgeons or pain specialists who’ve done plenty of these procedures. The more experience, the better. Ask about their track record.
Pick hospitals that have national or international accreditations like NABH or JCI. These seals of approval usually mean the place sticks to strict quality and safety standards.
Recovery doesn’t end when you leave the OR. Make sure the center offers device programming, rehab, and long-term follow-up. These should all be personalized to your needs.
Don’t just take the hospital’s word for it. You need to read real patient stories or ask to speak with someone who’s had the treatment. Honest feedback gives you a better idea of what to expect.
Medical Tourism Considerations
You’ll need a medical visa, so start that process early. Most hospitals help with the paperwork and make travel smoother for international patients.
The bigger hospitals often have guest houses right on campus or hotel deals nearby. It’s a relief to have somewhere comfortable for you and whoever’s with you during your stay.
International patient teams usually help with translation, travel plans, and all the little logistics. If you don’t speak Hindi or you’re new to India, these folks make a big difference.
Takeaway

Epidural stimulation gives hope to people with spinal cord injuries, but it cannot cure your condition completely. Some people see better movement or stability, maybe even improvements with blood pressure or bladder control.
Still, results depend on the type of injury, your health, and how dedicated you are to rehab. It works best if you stick to a steady training routine and keep your expectations realistic. Since this treatment means surgery, ongoing care, and a big price tag, you need a solid team of specialists who know what they’re doing.
If you’re thinking about this therapy, lean on trusted medical advice, pick reputable treatment centers, and plan for the long haul.
Considering epidural stimulation for spinal cord injury in India? MedicoExperts assists patients worldwide by coordinating consultations with top hospitals, experienced doctors, and advanced treatment centers. We also support you with medical visas, accommodation, travel planning, and complete documentation, making your treatment journey smoother and stress-free.
Frequently Asked Questions (FAQs):
Q1. Is epidural stimulation for spinal cord injury a permanent cure?
A. No, epidural spinal cord stimulation is not considered a permanent cure for spinal cord injury (SCI).
It can help restore voluntary movement, improve autonomic function (like bladder/bowel control), and support rehabilitation, especially when paired with intensive physical therapy, but it does not fully regenerate severed spinal cord tissue or permanently reverse the injury. Its benefits are generally contingent on ongoing use and rehabilitation.
Q2. How long does the epidural stimulation device last?
A. While specific device lifespans for epidural stimulation in SCI aren’t universally defined, similar spinal stimulation devices (used for pain and neuromodulation) typically have battery lifespans ranging from 5–9+ years, depending on whether the battery is rechargeable or not. These components are replaceable or removable through follow-up surgery when needed.
Q3. Can epidural stimulation help with chronic pain from spinal cord injury?
A. Yes, electrical stimulation of the spinal cord can help reduce chronic neuropathic pain in some people, much like other spinal cord stimulation therapies used in pain management. These implants modulate pain signals and can lower pain intensity, though response varies per individual.
However, the primary research focus for epidural stimulation in SCI today is often motor and functional recovery, not pain relief alone, although pain improvement may occur as part of overall neuromodulation benefits.
Q4. What is the recovery time after epidural stimulation surgery?
A. Recovery from the surgical implant typically involves:
(i) A relatively short hospital stay (sometimes same-day or 1–2 days)
(ii) Initial wound healing over 1–2 weeks
(iii) Gradual return to normal activities over several weeks
Many rehabilitation programs begin within days of surgery, although meaningful functional changes usually evolve over weeks to months with intensive rehabilitation and device programming.
Q5. Are there any risks or side effects in epidural stimulation for spinal cord injury?
A. Yes, implanting and using an epidural stimulator carries some risks. These can include:
(i) Infection at the surgical site
(ii) Device migration or malfunction
(iii) Pain or discomfort around the implant
(iv) Rare but serious complications (e.g., epidural hematoma or nerve injury), depending on individual circumstances
Most adverse effects are infrequent, and careful surgical technique plus follow-up reduces risk.
Q6. Can children with spinal cord injuries receive this treatment?
A. Research is ongoing, but not as established in children as in adults. Some neuromodulation techniques (like non-invasive spinal stimulation) show promise in pediatric SCI, and children may benefit due to greater neural plasticity.
But long-term data on implanted epidural stimulators in children is limited, and safety/efficacy must be assessed on a case-by-case basis with specialized pediatric care.
Q7. How is epidural stimulation different from other neuromodulation therapies?
A. Epidural stimulation (EES) involves a surgically implanted array of electrodes placed in the epidural space over the spinal cord to deliver targeted electrical pulses. It’s often combined with rehabilitation to help enable movement and restore function below the injury site.
In contrast:
(i) Transcutaneous spinal stimulation (tSCS) is noninvasive (electrodes placed on the skin).
(ii) Traditional spinal cord stimulation for pain targets dorsal sensory pathways to reduce pain, rather than stimulating motor circuits.
Epidural stimulation for SCI uses higher intensity and different stimulation patterns aimed at motor network activation, not just pain modulation.
Q8. Will I need to remove the device eventually?
A. Not necessarily. Epidural stimulation systems are designed to stay implanted long-term. However, you might need removal or replacement if:
(i) The battery runs out
(ii) There’s a device malfunction
(iii) Or it’s no longer beneficial for you
Devices can be safely removed or revised when necessary.
References
Relevant Articles For You
Traumatic Spinal Cord Injury Types
The purpose of the spinal cord is to transmit information between the brain and the body. If someone has a…..Read More
Spinal Cord Injury Complications
Are you tired of taking the help of someone to do your daily chores and are looking for a viable treatment solution to…..Read More
Acute Spinal Cord Injury Treatment
When nerves in the spinal cord are damaged, an acute spinal cord injury (ASCI) occurs. The impulses that are…..Read More
Recommendations To Understand Different Treatments
Stem Cell Therapy for Spinal Cord Injury
Spinal Cord Injury is one of the most common causes of long-term disability and this could also temporarily or…..Read More
Minimally Invasive Spinal Surgery in India
Spine surgery is a surgical procedure, mostly performed as the last retort to cure back pain. Typically, your…..Read More
Spine Surgery in India
Spine surgery is a medical intervention to address a wide range of spinal disorders, injuries, and conditions that…..Read More
Medically Reviewed by MedicoExperts Editorial & Clinical Review Board on 18 February 2026
Medical Disclaimer: This content is for informational purposes only and is not intended as medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare provider regarding any medical condition or dietary needs.




